Table of Contents
Symptoms of Plantar Fasciitis
- Morning heel pain when first stepping out of bed
- Sharp, sometimes stabbing or tearing sensation in the bottom of heel
- Increased heel pain with activities, prolonged standing, or driving a car
Causes of Heel Pain
- Flat Feet or High Arches
- Excess weight
- Tight calf muscles and tendons
- Activities that stress the foot such as running and jumping
- Shoes and/or sandals with inadequate support
Diagnosis
- Digital X-rays
- Ultrasound (Sonography)
- MRI
Conservative Treatments
- Orthotics. This is perhaps the easiest form of treatment. Orthotics are either “over the counter” or customized arch supports made for the individual to provide proper foot, heel, and ankle alignment. Many patients elect to buy Over the Counter Orthotics.
- Supportive Shoes. Ideally your shoes should bend near the toes, have a solid heel counter, and resist twisting/ deforming motion along the the shoe.
- Physical Therapy. Utilizing a combination of Electrostimulation, Therapeutic ultrasound, Hydrotherapy, Stretching, Massage, and Foot Taping will assist in reducing pain, inflammation, and propagate healing. This is instrumental in helping the patient regain function and return to normal activity.
- Corticosteroid Injections. Sometimes we may utilize injection treatment(s) to help reduce the pain and inflammation. Often it’s used in conjunction with other treatments and therapies giving you the best results.
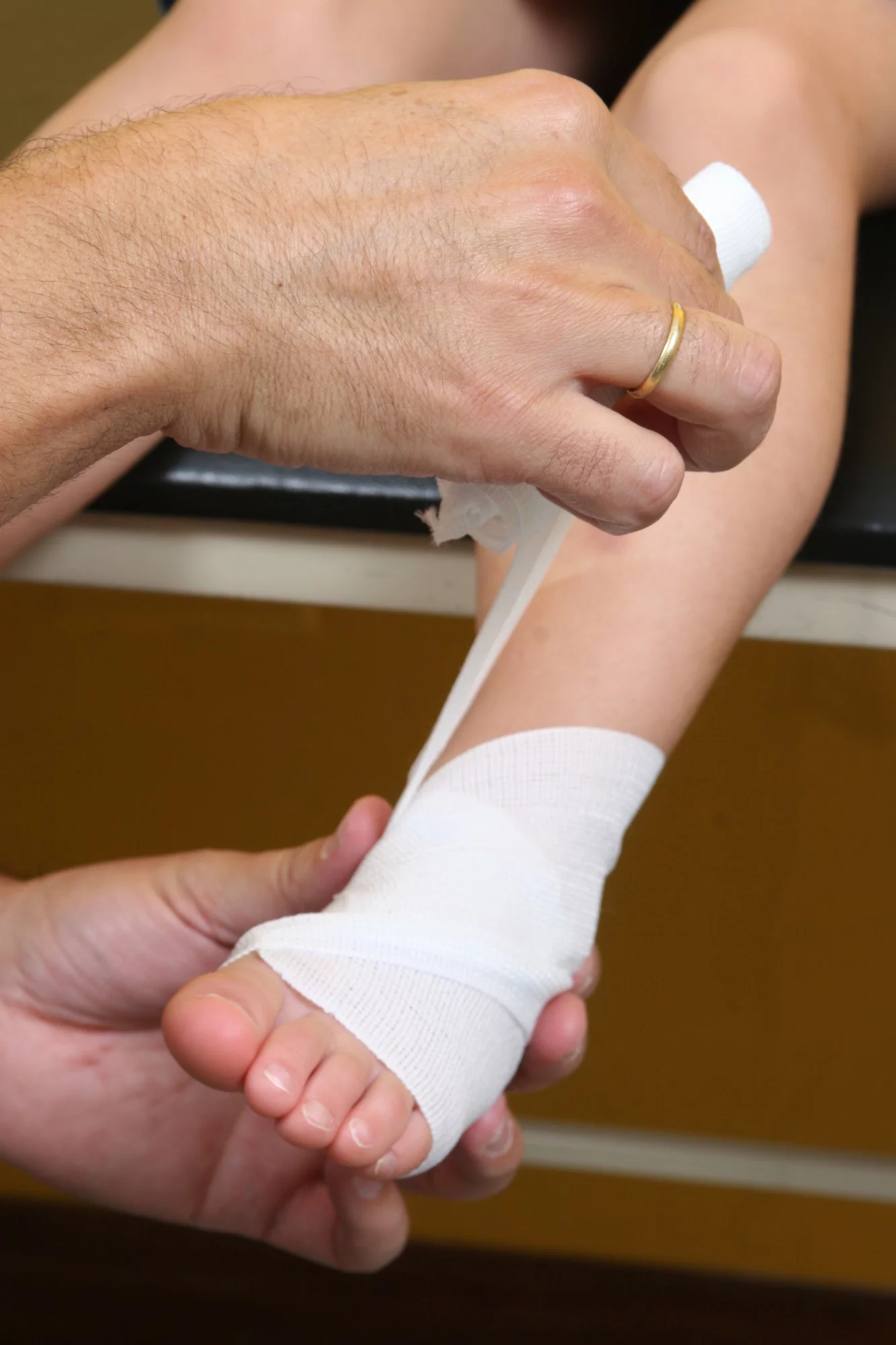
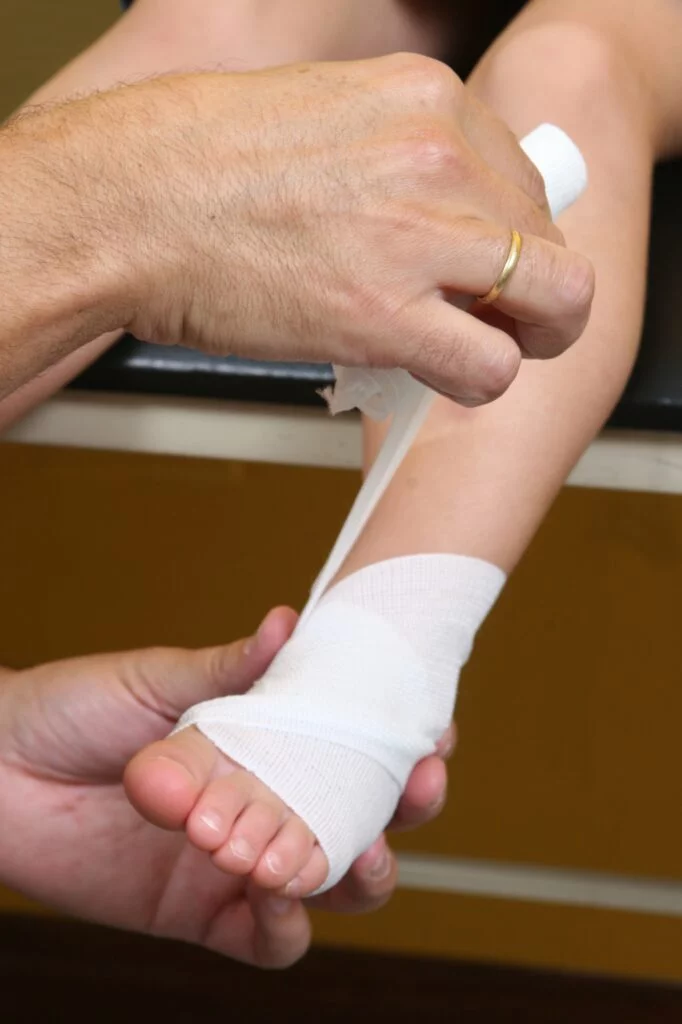
- Taping. We will tape the foot in such a way to protect the injured plantar fascia and restrict motion. In many cases, patients will learn to tape themselves. We recommend using KT Tape which is easily purchased online.
- Compression Therapy. Some patients respond to compression bandages and/or wraps.
- Night Splints. These are designed to be worn at night to passively stretch the calf, Achilles tendon, and arch during bedtime so there is reduced tension to the heel when the patient takes the first step in the morning or after rest. These devices are simple to use and very effective. You may easily purchase a Night Splint online.
Heel Pain Treatment in Orange County
If you are suffering from heel pain, feel free to contact our office or request an appointment online. Our podiatrists are experts in all areas of foot and ankle care, and will be happy to assist you with any problems you may be experiencing.